Questions and Answers on Cuboid Syndrome
Q: I find the biomechanics of the foot and ankle to be rather complex and difficult to learn, including the Type II pattern you describe. Can you please give me some suggestions?
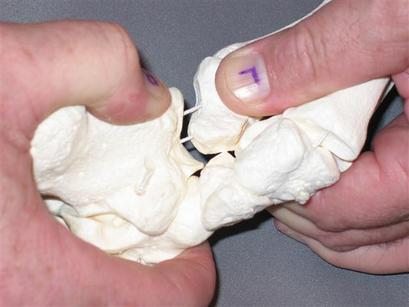
A: Yes, I would be happy to. I was very blessed to have owned a complete human skeleton very early in my career, and I often referred to it and the 3-dimensional nature of it made it so much easier to learn in ways that simply could not have occurred with 2-dimensional pictures in an anatomy test. Although cadaver dissection is part of our training, it is not the same. The dissection was long ago, the anatomy in my hand is real time.
I also purchased several foot models, left and right side of course and kept one of each intact and took the others apart. One I separated by major joints and the other I took completely apart. I enhanced the 3-D nature of the major joints by gluing window screen onto the articular surfaces so that the topographical nature was much more obvious. Looking at it from various angles and then stacking the other proximal bones - in essence – rebuilding the foot and ankle, and then inducing various motions was most helpful. In time I will post some of the photos of the enhanced topography.
Q: Can you briefly describe the 2 types of you mention?
A: Yes, I am guilty of naming the classical as Type I. It is a wonderful thing for clinician and client as it is painful and limiting, yet treatment is very easy, results are dramatic and long lasting. Typically 1-3 visits are all that are necessary. There are several examples in the literature. In Type I the cuboid is stuck in a manner best described as being whipped laterally about an anterior to posterior axis. The top of the cuboid is prominent, at least on the medial border. Inferior glide cannot be induced, nor can medial rotation. It is not unreasonable to describe the cuboid as being stuck in supination and treatment restores pronation.
What I call Type II is more complex and involves all of the major joints of the foot and ankle. Each joint loses a small amount of motion, so the forces are spread out and thus it is not always painful as is a Type I. However there will be some inhibition of muscular strength, endurance, balance and proprioception. There will also be a tendency towards a lateral ankle sprain as this pattern is basically a supinatory pattern and the person is unable to achieve functional pronation (not to be confused with excessive pronation). Functional pronation is the normal pronation that is part of the gait cycle, occurs in standing, etc. Type II are not always painful, many compensate fairly well without any gross gait deviation or pain. However, upon testing the joints, it is not unusual to provoke pain. From the standpoint of prevention these are worthy of treatment.
The typical motion losses are described in the separate link titled Cuboid Syndrome.
Q: Can you mention the motion restrictions in a Type II ?
A: They typically are:
Q: You say that a Type one takes 1-3 visits to resolve. Given the complexity of Type II, it must take much longer to correct?
A: Actually, most cases respond very quickly, within the same 1-3 visits. Of course the hands-on work takes longer as we are dealing with several motion restrictions as opposed to the “key dysfunction” of a Type I. The exceptions would be someone who has a true laxity that remains after you complete the mobilization.
Q: Please explain “key dysfunction”.
A: It is a borrowed term from Osteopathy. In this context, you may find several restriction throughout the foot and ankle, yet it is the cuboid restriction that is influencing them all. You could spend an inordinate amount of time chasing various hypomobilities and hypermobilities, but instead; addressing the cuboid resolves all of them. Hence the term “key dysfunction”. In Osteopathy, the term is actually “key lesion”.
Q: I thought that a person with a whether a Type I or a Type II had the problem due to preexisting laxity/hypermobility. However, you seem to imply the hypermobility and hypomobility coexist. Is that true?
A: Yes. It is important to distinguish between a true hypermobility and an apparent hypermobility. I had a severe true hypermobility when I completely tore my anterior talofibular ligament and the only lasting cure was surgical. There are lesser grades of true hypermobility due to stretched or partially torn ligaments that take longer to heal. Rehabilitation time of course is longer. The hypermobility has to be dealt with directly.
In contrast an apparent hypermobility is one that tests as hypermobile, yet it is a mutable property. Upon restoring mobility in the various directions that the major joints are restricted, the hypermobility is no longer detectable. This is because it was positionally induced and upon restoring normal position and reolving the hypomobilities, the hypermobility also resolves. In essence hypermobility and hypomobility are on opposite side of the midline of the bell curve. Both move towards the mean (regression to the mean) when the hypomobility is treated. You will also find dramatic and quick improvement in muscle function, balance and proprioception. In essence, the hypermobility is dealt with indirectly, specifically; by addressing the hypomobilities.
Q: How did you discover the Type II ?
A: I do not recall a specific eureka moment, but I always had a penchant for seeking out patterns, rather than just focusing on the symptomatic structure. I learned very early on that the body has to adapt and compensate for injuries and in time those other areas can become symptomatic. Even before going to PT school I plumbed the depths of Osteopathic Manual Medicine, and that undergirds this pattern seeking.
Q: How many bones are in the foot and ankle?
A: Ignoring sesamoids, which are small “pulley” bones that do not form true joints, there are 28 by my count.
Q: How many joints?
A: By my count, there are 30.
Q: 28 bones and 30 joints?
A: Ooops, no, I goofed. I failed to count the articulation between the 2nd & 3rd, 3rd & 4th, and 4th and 5th metatarsals, so 33?
Q: Are you counting all of the facets between the calcaneus and talus as one joint?
A: Yes.
Q: Can I come and have you evaluate my foot and ankle?
A: I would be happy to, send me an email at mailto:info@heschinstitute.com
Q: Do orthotics help with Type I and Type II ?
A: Somewhat. The type I and II are typically only on one side of the body, right more often than left. Rarely, does it occur bilaterally. So yes an orthotic can control position and mobility to some degree. However, the primary influence of an orthotic is in the sagittal (side view) and frontal (front and back view) planes and much less so in the transverse plane. Thus it is very helpful to have hands-on joint mobilization in addition to orthotics. When I see a client with a Type I or II on one side and they come with 2 distinctly different orthotics I compliment the person who provided them. However, upon restoring functional motion, the orthotic typically does have to be adjusted. Philosophically, I believe it more important to restore the motion potential that a person has, rather than depend on an external device (orthotic) alone. When I see the same orthotic on 2 different foot/ankle presentation, I am a bit reticent to comment. However, as soon as motion is balanced, the orthotics are then rendered more appropriate.